Home » Cornea » Corneal Transplants
Corneal Transplants
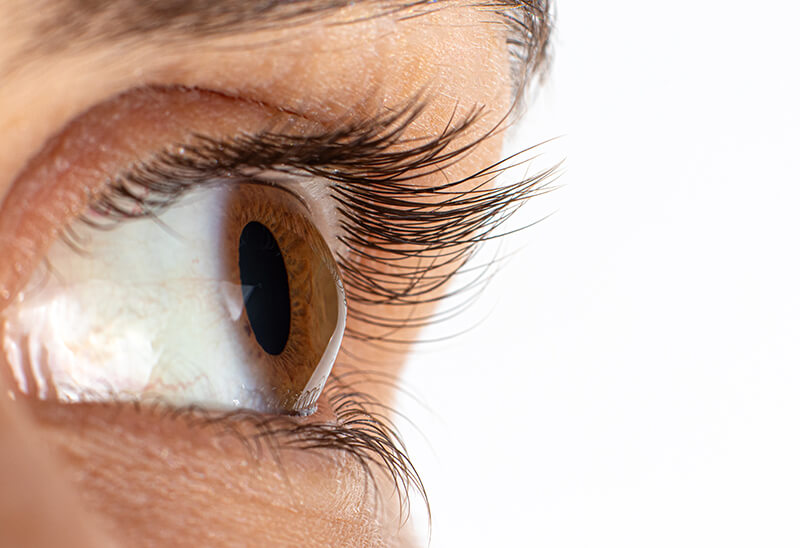
The cornea is the eye’s outermost layer. It is the clear, dome-shaped surface that covers the front of the eye. It can be described as being like a window onto the interior of the eye. If the cornea is injured, it may become swollen or scarred, and its smoothness and clarity may be lost. Scars, swelling, or an irregular shape can cause the cornea to scatter or distort light, resulting in glare and/or blurred vision. A corneal transplant is surgery to replace the cornea with tissue from a donor. It is one of the most common transplants done.
Corneal transplantation is recommended for people who have:
- Vision problems caused by thinning of the cornea. This is called keratoconus.
- Scarring of the cornea from severe infections or injuries.
- Vision loss caused by cloudiness of the cornea. This is called Fuchs’ dystrophy.
- Rejection of a previous corneal transplant
A corneal transplant is also known as a keratoplasty or penetrating keratoplasty (PKP) involves replacing an eye’s scarred, diseased or damaged cornea with clear corneal donor tissue. This procedure can improve visual acuity as it is replacing the cloudy cornea with clear donor tissue.
The donor cornea is prepared to create the corneal “button.” The corneal button will become the transplanted cornea. The diseased, or scarred, cornea is then removed, creating a “bed” for the transplant cornea. Finally, the donor cornea is gently sewn into place with ultra-fine sutures (approx. one-third the thickness of human hair, or less). Stitches are typically removed at one year.
Postoperatively, patients should expect very gradual recovery of vision. In fact, the best vision may not be obtained for six to 12 months or more following surgery, even though vision may be improved from the first day after surgery in some cases.